When I was 19 years old, I was hit by a car while crossing the street. I flipped over the hood of the car twice before landing on the asphalt, shattering my right side. I sustained my most serious fractures in my humerus, but I also fractured my hip, my fibula, and my ankle. It took me two years to fully recover and regain 90% of my mobility, along with some of — but not all of — my pre-accident strength.
I often explain my life story in terms of this event and emphasize how I went from nondisabled to disabled in this one moment. The truth is more complicated.
I first learned the term “covering” as I entered my diversity, equity, inclusion, and belonging career. I couldn’t quite differentiate what it meant from passing — which is physically representing yourself as a member of the dominant group — so I looked it up. I found Kenji Yoshino’s excellent 2006 New York Times article, “The Pressure to Cover,” and at the same time, found a word to describe myself.
Covering is downplaying a nondominant identity. Whether that means changing your last name to seem less like a marginalized racial or ethnic identity, keeping images of your partner of the same gender identity out of your office to downplay your sexual orientation, or powering through major medical issues to ensure others don’t see your disability as “getting in the way,” covering is not about hiding your identity, but instead, making it less obtrusive.
Since I was 15, I had been managing a seemingly ever-growing list of chronic illnesses from hypothyroidism to polycystic ovarian syndrome (PCOS). In my twenties, after developing severe congestion, fatigue, migraines, and various stomach disorders, I learned after seeing multiple specialists that I had benign paroxysmal positional vertigo (BPPV), severe mold allergies, a chronic stomach condition, and surprisingly, a heart murmur. I learned of the murmur just a few months after my paternal grandmother had a heart attack that revealed she had valve disease, to which I now know I am predisposed.
It was in reading Yoshino’s account of his own experiences that I learned that I had been covering for years.
After my car accident, I never once described myself as disabled or having a mobility disability. In the hospital before my surgery, my doctor advised me to take a three-month leave of absence from college. I resisted, and I returned back to school one week after my surgery.

I went into extreme planning mode, contacting the university myself to arrange for shuttle services to and from campus knowing that I could not walk that distance under the best circumstances, let alone in the dead of an icy winter. I requested reasonable accommodations to bring my iPad and keyboard to class so I could type notes since I could not use my right arm. I contacted my professors and let them know I would be in their classes.
When one professor stated that she’d rather I not take her class and focus on my recovery because she worried I would not be able to “keep up,” I dropped her class and begged a human rights professor teaching a class at the same time to make an exception and let me join. I also vowed that I would perform better, be sharper, and just generally excel. That first professor’s rejection galvanized me; I would not “disappoint” anyone during my recovery.
Not once did I consider that I may live with mobility-related disability for the rest of my life. I couldn’t even consider it an option. Based on the cultural messages I had been learning my whole life, I believed that being disabled made you less than, invisible, pitiable, and weak. It’s part of why I became obsessed with diagnosing and systematically eliminating my chronic illnesses long before my accident, and truthfully, long after.
I grew up with the term “invalid,” meaning a person who is sick, disabled, and bed-ridden. I also grew up with its homonym (two or more words with the same spelling and different meanings), “invalid” meaning being without, wrong, unrecognizable, and void. The two words came to mean one and the same to me.
I wanted to be strong, high-performing, and respected. The idea that a person could be all of those latter things and disabled seemed impossible, a contradiction.
So, from my teens on, any time I had chronic symptoms, I pleaded with my parents to take me to multiple doctors and specialists. I wanted a diagnosis, a treatment plan, and a pathway to full-scale eradication of any illness I may experience. For surface-level issues, this worked.
I’ve spent more money on eliminating visible symptoms of my polycystic ovarian syndrome than just about anything other than my house. Expensive dermatologists, skin treatments, and cosmetics to eliminate hormonal acne, personal trainers and extreme dieting to shed weight, and invasive treatments to eliminate the more noticeable effects of stomach cramps, back pain, and hormonally-driven changes in mood.
I was proud any time someone said they were “shocked” that I had PCOS and questioned whether I wasn’t borderline, someone who just had a few symptoms but had a mild case.
The fact that I would frequently pass out from stomach pain was something that only my inner circle knew. It may not be totally possible to pass — unexpected fainting spells, vomiting, temporary loss of vision, debilitating migraines, and even an inability to reach for or lift items — meant that people knew, abstractly, that I had some “health issues.” But they were issues, not a condition to them.
And that’s what I wanted. In some cases, I wore my discipline and resolve to act in spite of these issues as a badge of honor.
In my first truly high-pressure job, I found myself in a meeting about the organization’s future vision. Excitingly, I was asked my opinion on long-term strategy for the first time. I was also overcome with the need to vomit. I briefly excused myself, and knowing I couldn’t make it to the coworking space’s bathroom, found an oversized, bucket-like trash can to throw up in. I wiped my face with a wet wipe, swallowed some water, and reentered the meeting.
The one setback was that the entire office and conference room were encased in glass, meaning the other meeting members had seen the whole situation. My boss asked if everything was okay or if I needed to go home. I brushed off the incident and kept going.
At that same job, I started to feel the onset of a monster migraine. I developed almost immediate light sensitivity, colored spotting in my vision, and skull-wide pressure. Aware that in my short, three-year career I had not once taken a sick day, I panicked. There was no way I was going home early. That would be a sign that I couldn’t “handle” my job, and I would never concede that kind of defeat.
I asked a colleague for ibuprofen and was supplied with two tabs of extra-strength Excedrin. I didn’t think to check the ingredients before I swallowed them, not realizing that Excedrin contains caffeine, which is a high-risk substance for someone with vertigo. Within about half an hour, I found myself experiencing a massive vertigo attack, almost falling directly over. I crawled under the dark space below my standing desk, lowered the brightness on my computer, and kept typing. My two interns had prepared a presentation for me that day, and without questioning, printed out the presentation, sat on the floor next to me, and led it.
It took hours before I was able to stand, and I had to take a Lyft home because I couldn’t walk. The next morning, when I got out of bed and tried to stand, I fell directly over, face-first onto my wood floor. I made an appointment with a doctor to re-up my prescription of Meclizine and found a physical therapist in my office building to help manually by performing the Epley maneuver.
Years later, one of the interns who was there that day noted that he had never met anyone more hardworking than me. I took it as a compliment, the way he meant it, but I felt some ambivalence. I couldn’t even remember the work I did that day. I can’t really remember much of what that job was; but, I can easily relive the anguish of feeling trapped under my desk, not knowing if the dizziness, nausea, or inability to move would ever go away.

Disability activist Alice Wong’s work on disability visibility set me on a fundamentally different trajectory when it comes to identifying my disability, not as something that should be covered, but something to be discussed and considered. Through reading her work and the myriad stories of disabled people she has platformed, I have come to realize that it is not my obligation to “power through,” but that workplaces should be making space and accommodations for the 26% of Americans that live with disabilities.
Paid sick time, generous and paid leave, healthcare coverage, flexible work schedules, accessible buildings, and access to necessary tools and equipment must be the baseline. Ingrained biases and negative attitudes towards disabled people, too, must be deprogrammed in our offices.
Some of this work begins with deprogramming the internal beliefs many disabled people hold about ourselves. But to focus only on personal responsibility is disingenuous, manipulative, and callous. These beliefs exist in many disabled people, myself included, because they are taught to us by the people around us.
I have had bosses, clients, and well-meaning colleagues tell me my “health comes first” and at the same time ask me for a favor or to work on something they need. Which is it? Does my health come first, or does the task you want me to do? These same people are often the first to say, “you just focus on getting better,” as if whatever I am managing is treatable or that I would even want to treat it. Perhaps most irksomely, I often hear them say that the reason I am ill is because I work too much, stress too much, do too much, and I don’t know how to relax.
The last one hurts the most because there is truth to it. Until the beginning of 2020, I put my mind and body through such extreme working hours that I stopped producing my own adrenaline and developed severe issues producing and regulating my cortisol levels, along with other stress hormones. Yet, I refuse to take the blame for that alone. I had my reasons.
Healthcare is extremely expensive, especially when you have chronic conditions and rarer illnesses that not every doctor has a playbook to address. I worked two full-time jobs for the first two years out of college in part because I couldn’t fully afford medical care otherwise.
Plus, covering is expensive. It meant having to freelance, work extra jobs, and scrimp and save in other parts of my life that might lead to more sustainable health practices. I made less than $50,000 a year when I was seeing dermatologists, personal trainers, nutritionists, and physical therapists, all to look less sick. I believed, and not wrongfully so, that if I didn’t maintain the appearance of a healthy working professional, I would never be successful.
This was reinforced by the colleague who reminded me when I turned 24 that I was lucky to be married because women were no longer viable after the age of 25. The thought that came to mind was simply, how many years of viability do I lose as a chronically ill person? And what do the keloid scars and moderate restricted right-side mobility subtract? Was I ever viable?
The answer is, of course. I was viable then, now, and for all time. Yet, that idea isn’t always front and center for me, even now after years of therapy and support from the disability justice community.
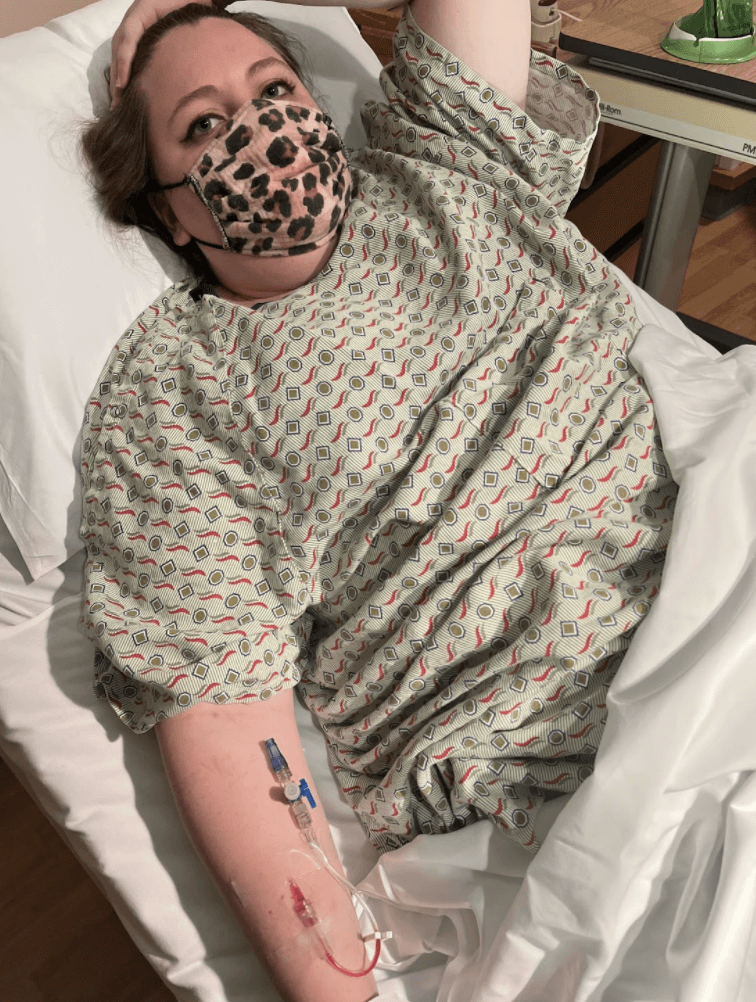
Two weeks ago, I went to the emergency room for complications related to my pregnancy. The truth is, my pregnancy has been very difficult, and routine visits to the hospital (not just my obstetrician) are a big part of the experience. I am surrounded by people telling me something must be wrong, that my symptoms will go away, and that I must not be doing “all the right things” if I feel this sick all the time.
Well, I am in the “golden time” of my second trimester, and I feel worse than ever. Importantly, my doctor says that while unfortunate, this is normal. Many pregnant people have such severe pregnancy symptoms they are unable to work or function; still, others end up at the hospital for weeks at a time. Having preexisting chronic conditions doesn’t necessarily mean your pregnancy will be tougher on your body, but in my case, it has. Migraines that used to last 36 hours now last 6 days, nausea that came on with vertigo attacks now persists almost every day starting at 4:00 pm onward, and chronic muscle and joint pain has accelerated to some of the highest levels I have ever experienced.
And… I am running a growing business that has a payroll for ten employees to support. The pressure of that responsibility looms large every day of my life.
When I came home from my stay in the ER, I worked for two hours on a client project that team members were handling for me while I was away. I wanted to make sure no balls were dropped, but I also really, really, really didn’t want to ask them for more help than what I deemed “reasonable,” for fear they would feel I was taking advantage of them. The next day, I led three facilitated sessions, working about eleven hours, owing in part to the fact that we had no available substitutes. This did not square with the on-call doctor’s recommendation to take it easy, avoid stress, and rest.
The unlearning process is difficult. Perseverance, discipline, and effort have always been the characteristics most emphasized to me as a worker and an American. Unlearning is even harder when faced with everyday social pressures. Some of my clients are lovely and understanding, especially since I became pregnant, either owing to their personal experiences, their empathy, or their ongoing struggles around retention because of the great resignation of working parents. It’s worth noting that not all of them are.
Despite vulnerably and candidly naming that I was slow to respond to email because I was in the ER, one client told me I should have handled the situation by escalating any scheduling concerns to them before I went to the hospital. Another asked after my health and then affirmed that our contract had a very specific delivery date defined.
The easy answer would be to drop the clients who don’t understand. And arguably, in our current market, that is an option. But it won’t always be.
In 2021, the pressure to cover mental health issues is especially troubling. While employees are talking more about these issues, they are still working longer hours than they did pre-pandemic. According to Mental Health America’s 2021 State of Mental Health in America, 19% of people in the U.S. are living with a diagnosed mental health condition nationwide, 1.5 million more than in 2020. COVID-19 has killed many and infected many more, with the long-term effects still unknown. The infectiousness of the disease has limited social support for childcare, elder care, and community help, taxing caregivers.
In 2006, Yoshino wrote about covering and some of the groundbreaking civil cases that were helping address social stigma. Fifteen years later, and the picture doesn’t look so different. The question, then, is clear: How can we change social attitudes and biases around disability (and all other marginalized identity groups) before we dig ourselves deeper into this hole?
Significant policy changes, a stronger social safety net, reprioritization of workers over shareholders, and ongoing, social identity-specific education are all at the top of the list.
But how about we try this to start: before assuming or advising, seek to understand others first. My pregnancy may not be like the one you experienced, just like my ability to cover in the first place may be a privilege you have never had. Let’s focus on eliminating “should” from our vocabulary and instead consider asking people to share who they are with us.

